Table of Contents
What Is Ehlers-Danlos Syndrome?
(EDS) is an inherited connective tissue condition characterized by hypermobility and fragility of the joints and other connective tissues. This article will review the classifications, symptoms, diagnosis, and comprehensive treatment options available for individuals with Ehlers-Danlos Syndrome including neuromuscular based Physical Therapy and Regenerative Medicine using Platelet Rich Plasma (PRP), Bone Marrow Stem Cell, and Dextrose Prolotherapy injections for joint stabilization, and ligament strengthening.
Ehlers-Danlos Syndrome Symptoms
Ehlers-Danlos Syndrome is associated with various genetic disorders of collagen synthesis, which ultimately may have effects on diverse tissues including the skin, joints, heart and vascular system, as well as other internal organs. Patients with Joint Hypermobility Syndrome associated EDS will often present with frequent sprains, multiple joint subluxations and dislocations, early joint structural degeneration, and diverse issues including low blood pressure, fainting, skin fragility, varicose veins, bursitis, tendinitis, stretch marks, digestive and immune system issues, spine pain, and chronic joint instability leading to multi-site pain. Patients with Ehlers-Danlos Syndrome are frequently mislabeled or misdiagnosed for years. Once an experienced practitioner properly identifies the underlying cause of their pain and dysfunction, the individual with EDS can embark on a road to improved management and a higher quality of life.
How Is Ehlers-Danlos Syndrome Diagnosed?
As greater understanding of the characteristics involved with hypermobility have been researched, the diagnostic criteria have become complex. The Ehlers-Danlos Society has published guidelines to better categorize the different types of EDS. Table 1 (see below) outlines the 2017 International Diagnostic Criteria for EDS based on distinctive genetic differences and functional characteristics. The different types vary based on the type of collagen that is dysfunctional, the degree of skin and subcutaneous tissue involvement, the degree of heart and vascular involvement, the degree of involvement of internal organs and structures such as the colon, uterus, veins and arteries, whether there is eye (lens or cornea) involvement, muscle tone / weakness, and abnormal spinal curvature. Genetic testing may help to classify the particular form of EDS that affects each patient.
Presence of Abnormal Collagen
Many different mechanisms have been shown to lead to abnormal collagen structural integrity. The type of collagen is determined by DNA encoding and inherited genetic mutations lead to different characteristics within the collagen tissue formed. Variation has been found within the design of the protein structure, the folding and cross-linking of the protein fibers, dysfunction of the muscle and collagen matrix material, abnormal biosynthesis of glycosaminoglycans, defects in the complement pathway, and disorders of intracellular process.
Autonomic Nervous System Function
The autonomic nervous system regulates multiple processes within the body including heart rate, blood pressure, breathing, and digestion. The excessive elasticity of the veins causes blood to pool in the lower extremities in patients with hypermobility syndrome. The body may compensate for this by producing extra epinephrine / adrenaline to stimulate a more normal blood pressure, and this may result in excessive anxiety, nervousness, sweating, diarrhea, nausea, lightheadedness, and hypersensitivity to stimuli. Chronic fatigue may result from this over-driven and sympathetically up-regulated autonomic nervous system condition.
Types of Ehlers-Danlos Syndrome
Table1: EDS Types Chart (Reproduced from the Ehlers-Danlos Society)
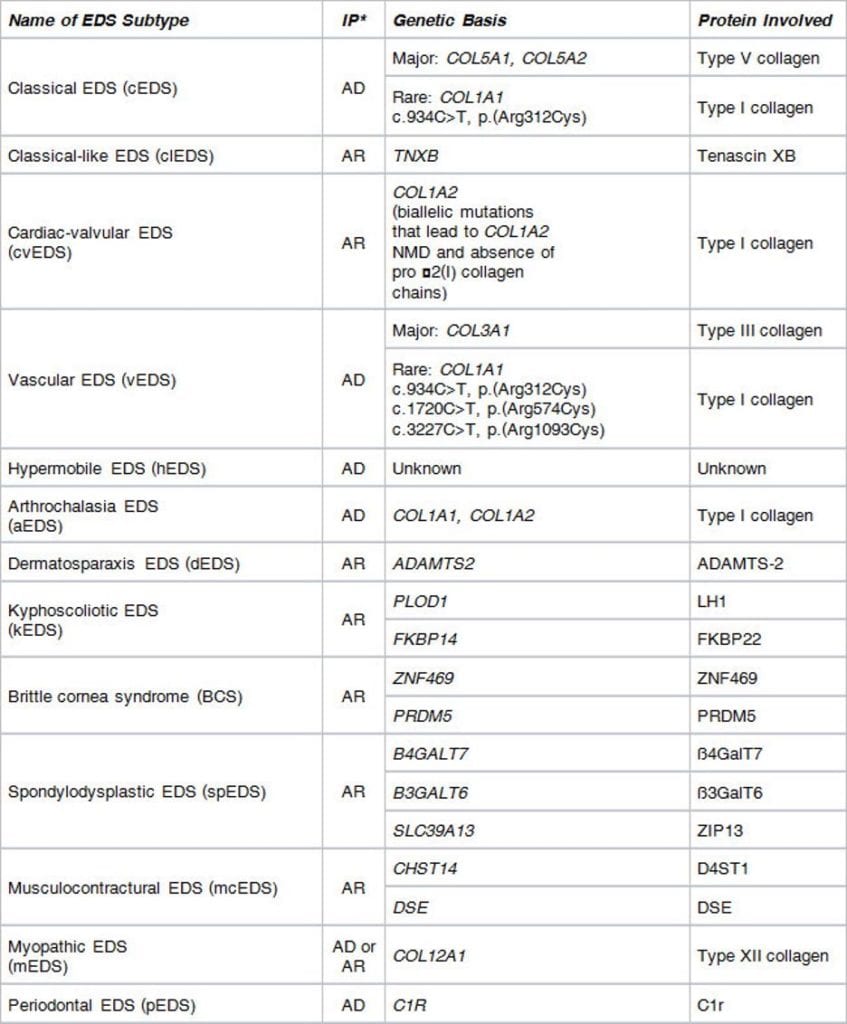
* Inheritance Pattern: AD = autosomal dominant; AR = autosomal recessive
Postural Orthostatic Tachycardia Syndrome (POTS)
POTS is a condition in some patients with EDS present which can include frequent periods of fainting, dizziness, and low blood pressure. This is thought to be due to excessively elastic collagen structure supporting the heart, arteries and veins. The blood pressure “pulse” from the heart is dissipated throughout the arterial system such that the blood pressure remains low. In addition, the highly elastic veins do not pressurize the blood volume to return it to the heart sufficiently. Treatment options for this include adding salt to the diet along with more fluid intake, avoidance of caffeine, alcohol and diuretic medications which deplete body fluid, use of support compression stockings for the legs, avoiding prolonged standing, “calf-pumping” (exercising your calf muscles to push the blood volume back up to the heart), and periodic elevation of the legs and feet. Sometimes medications may be needed to increase blood volume or blood pressure, such as Hydrocortisone (Cortef) or Fludrocortisone (Florinef) to retain fluid, and/or Midodrine to increase blood pressure.
Criteria: Hypermobility Ehlers-Danlos Syndrome (hEDS) vs. Hypermobility Spectrum Disorder (HSD)
Some individuals with EDS simply have joints that move beyond their normal limits compared to other individuals, and may not manifest other major signs and symptoms of significance outside of joint instability. These patients would be considered to have Hypermobility Ehlers-Danlos Syndrome, also known as “Type 3 EDS”. Hypermobility Spectrum Disorder defines patients that have a greater degree of severity with more negative impact on their quality of life and activities of daily living. The specific joints that are involved, the presence or absence of other musculoskeletal conditions, and the Beighton scoring system help to categorize patients within the Hypermobility Spectrum Disorders. Joints often become more restricted with the natural aging process.
The Beighton Score and The Brighton Criteria
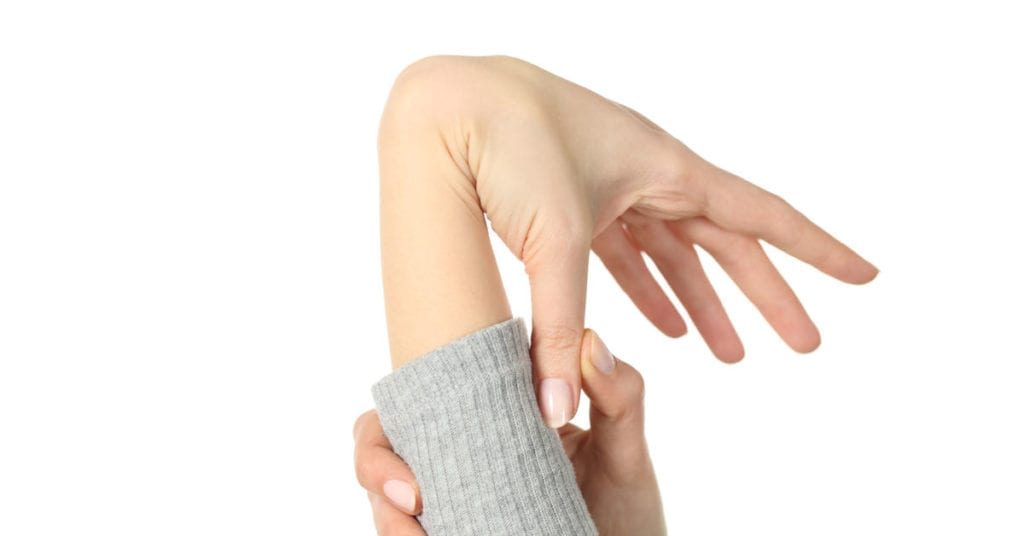
The Beighton Score is a 9-point scale assigning 1 point for each of the following joint motion abnormalities:
- Bending your little finger back further than 90 degrees (1 point per side)
- Bending your thumb forward to tough your forearm (1 point each side)
- Hyperextending your elbows beyond a straight line (1 point per side)
- Hyperextending your knees beyond a straight line (1 point per side)
- Putting your palms flat on the floor without bending your knees (1 point)
The Brighton Criteria uses the Beighton Score (each spelling correct) in addition to other characteristics to help further diagnose the patient’s degree of severity. The Major and Minor Criteria outlined below help to score the patient’s condition. Diagnosis for EDS requires either 2 Major Criteria, 1 Major and 2 Minor Criteria, 4 Minor Criteria, or 2 Minor Criteria and an unequivocally affected first-degree family member.
The Major Criteria to meet the diagnosis of EDS are a Beighton Score of >4 and joint pain for longer than 3 months in 4 or more joints.
The Minor Criteria include a Beighton Score of <4, arthralgia (pain) for more than 3 months in 3 or fewer joints or the low back, lumbar spondylolisthesis or spondylosis, joint dislocation/subluxation in more than 1 joint, the presence of soft tissue conditions such as tendinitis or bursitis, stretch marks on the skin, thin hyperextensible skin, abnormal scarring, drooping eyelids, myopia, Marfinoid body shape (tall, slim, excessive finger length), varicose veins, hernia, rectal prolapse, uterine prolapse, or mitral valve prolapse.
EDS Treatment Options
The traditional non-invasive treatment options for patients with Ehlers-Danlos Syndrome and hypermobile joints include many standard options used for chronic pain and joint dysfunction. Many of the typical options will produce gradual improvement and compensation strategies for the condition but the limitation caused by the excessively elastic ligaments and joint connective tissues will often lead to some level of frustration for both the healthcare provider and the patient. Emotional and physical setbacks are common.
Chiropractic manipulation may be helpful for symptomatic relief but often the joint mobilization will result in only short or intermediate term pain reduction. The ligamentous support that is the root cause of the dysfunction is generally not improved or eliminated by these types of therapeutic interventions. In fact, excessive manipulation might worsen the already elastic collagen tissue and joint hypermobility.
An appropriate general fitness program may help the patient to attain more self-reliance and improve their muscular strength. A focus on increasing joint and musculoskeletal flexibility through aggressive stretching, such as extreme postures during yoga, may actually result in even greater joint structural laxity. Excessive exercise beyond the strength of the connective tissues may lead to increased pain, joint inflammation, or tissue injury and should be avoided.
Physical Therapy
Physical therapy using a wide variety of graded exercise prescription, manual therapy, massage therapy, modalities for inflammation and pain management such as the Class IV Laser pictured here, as well as biofeedback are often offered to individuals diagnosed with Ehlers-Danlos Syndrome. Education around proper body mechanics, postural correction, optimizing ergonomics, and pelvic, spine, and extremity support can assist in reducing joint strain and injury. Specialized Physical Therapy using methods focused on the improvement of neuromuscular control and muscle balance can improve joint stabilization and decrease pain.
Redcord Neurac: Therapy Focused On Neuromuscular Control
In our practice we find EDS patients frustrated at times with their ability to tolerate and see benefit from conventional physical therapy interventions. The use of closed chain suspension exercise can facilitate agonist, antagonist, and synergist muscle activation around the weight-bearing joints improving stabilization. Use of the Redcord Neurac system gives a trained therapist the ability to off-load a graded percentage of the patient’s body weight creating an exercise that integrates multi-segmental core control while continuing to challenge joint stabilization with extremely low load or strain to individual joints. This system can provide the individual with EDS who is struggling to tolerate conventional exercise an option to improve strength and joint stability in a controlled, pain free environment with the goal of increased body awareness and a safe transition to a community fitness program.
NEUBIE - Neuro-Bio-Electric Stimulation: Addressing Pain, Anxiety, and Fear
Ehlers-Danlos Syndrome and the wide spread physical manifestations that it brings can take significant emotional and social tolls as well. Stress is accumulative and our bodies can only take so much whether the stress is physical, emotional, nutritional, or psychosocial. When these life stressors build, our ability to handle the next stress becomes more limited. The nervous system becomes less resilient and more sensitive as one lives in more of a sympathetically up-regulated autonomic nervous system state as discussed earlier. This often manifests itself is difficulty sleeping, digestive issues, muscle tension, anxiety, difficulty concentrating, immune system compromise, and a heightened pain response.
In the individual with EDS it is common to see more fear around movement due to instability and altered proprioception within the connective tissues of the joints. As an individual limits the variety of movements they make, they compensate further, move less, weaken, and movement becomes more fearful and threatening.
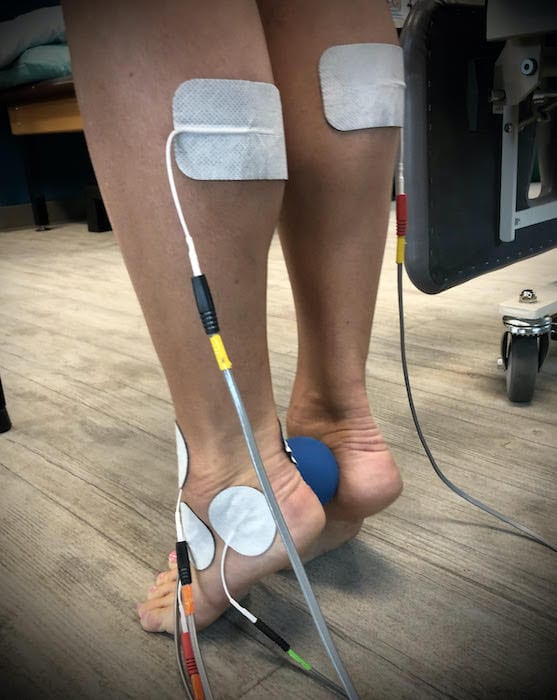
The NEUBIE – NEUro-Bio-Electric stimulation and the NeuFit Method uses direct current (DC) waveforms that are recognized by the body as its own. Using a scanning process a trained therapist can quickly identify areas of the nervous system that feel threatened. These areas of limited output (weakness / inhibition) or protection (guarding / tension) present in the neuromuscular system can then be treated using prescriptive frequencies that either release or increase tone in the muscles improving control and stability of the joints in the individual with Ehlers-Danlos Syndrome.
The NEUBIE also has a powerful protocol to treat the entire nervous system using the direct current Master Reset. The goal of this treatment in the individual with Ehlers-Danlos Syndrome is to improve the resiliency of the nervous system as a whole, so that the next stressor is not seen as threatening. After a few treatments with the Master Reset, we commonly hear reports of improved sleep patterns, digestion, decreased anxiety, and decreased pain.
Splinting And Bracing
Patients with hypermobile joints may benefit from the use of bracing and / or orthotic devices. These can reduce excessive motion and help to stabilize the joints with the goal of reducing the risk of subluxation, dislocation, joint injury, and pain. These can be custom-designed or purchased off-the-shelf and may help preserve the joints to some degree. Unfortunately, these are often heavy, inconvenient, and may require assistance to don and doff the devices. The skin contact may rub the skin excessively, which is already frequently fragile, and this may lead to open sores and chafing. Choosing a softer, more neuromuscular-focused support can be helpful in improving the muscle balance and proprioceptive input around the joint providing dynamic stabilization without gross mechanical restriction of joint motion. Kinesiotaping and neuromuscular bracing can be a beneficial initial approach to conventional bracing or orthotics.

Mobility Devices And Home Modification
The individual living day to day with Ehlers-Danlos Syndrome may find some days significantly more difficult than others. Having options of devices that can improve independent mobility, off-load joint strain, conserve vital energy, and provide modifications for the necessary activities of daily living is extremely important. These equipment options and environmental modifications can assist in maintaining safety and autonomy making those harder days more manageable, independent, and lower the risk of joint injury or falls. A physical and occupational therapist experienced in the treatment of EDS patients and their wide variety of physical and biopsychosocial issues can be very helpful for long-term positive outcomes and successful self-management.
Medication / Supplement Options
The joint and musculoskeletal pain that accompanies EDS may be improved with medication, with limitations due to addiction and side effects inherent in chronic use. Opiate pain medications will generally lead to tolerance and addiction and thus should be used only in severe, challenging cases. Opiate medications may cause or worsen digestive concerns, including nausea and constipation. Opiate medications may also worsen symptoms such as dizziness, lightheadedness, and fatigue.
Non-Steroidal Anti-Inflammatory Drugs (NSAID’s) are also a balance between benefits and risks. These can cause nausea, internal bleeding and kidney failure. These medications cause the reduction in the collagen tissue repair process because these medications inhibit collagen protein synthesis and interfere with articular cartilage production and repair. Since the primary concern in the EDS patient is fragile and elastic collagen, these medications can create even more problems for the EDS patient than in the non-EDS patient.
Over-the-counter vitamins and supplements are marketed to help with connective tissue health but there have not been high quality studies proving benefit for the EDS population. Generally, Vitamin C, Vitamin D3, and Vitamin K2 are essential for connective tissue and bone health. Methyl Sulphonyl Methane (MSM) and silica are helpful for collagen synthesis. Other cofactors that are considered helpful include zinc, calcium, magnesium and Co-enzyme Q10.
Surgical Options
The excessive collagen tissue fragility and elasticity present in the individual with EDS can create many challenges with typical joint and sports-related surgical procedures. The tissues often do not heal well after surgical repairs, such as with tendon repair using anchors and sutures, and there is a greater frequency of orthopedic surgery failure in this population. The surgeon needs to be acutely aware of the special needs of the EDS patient and compensate for this during surgery to try to reduce the probability of future joint surgery failure.
When the joints become severely degenerated, joint replacement may be recommended, especially for the knee, hip or shoulder. However, surgical joint replacement requires a strong supportive and flexible ligamentous capsule to hold the joint hardware in place, so individuals with Ehlers-Danlos Syndrome are more likely to dislocate after joint replacement and to need subsequent joint revision surgery. One should seek the expertise of a surgeon with experience dealing with the collagen tissue weaknesses inherent in EDS.
A final salvage surgical option for a failed joint could include joint fusion, in which the two bones are joined together to eliminate all motion at the joint, which will unfortunately usually produce additional, excessive stress on the surrounding joints, leading to premature failure of these nearby adjacent joints as well.
Platelet Rich Plasma and Prolotherapy Injections
This section discusses the use of Regenerative Medicine injections including Platelet Rich Plasma, Bone Marrow Aspirate Concentrate, and Dextrose Prolotherapy for the treatment of joint instability and connective tissue degeneration in the individual with Ehlers-Danlos Syndrome. Platelet Rich Plasma (PRP) is a more advanced and well-known form of a technique known as Prolotherapy.
Prolotherapy is a treatment option that has been proven for over 80 years to strengthen ligament weakness, improve the stability of hypermobile joints, and generally reduce pain. High-resolution ultrasound and MRI studies have proven that there is stimulated connective tissue growth and repair of degenerative tissues and joints. Prolotherapy has been shown in an animal study by Dr. Lui to increase ligamentous mass by 44%, ligament thickness by 27% and the ligament-bone interface by 28%. Double-blind studies in humans have demonstrated joint stabilization and correlated this with patient outcome improvement.
Prolotherapy has proven to be cost-effective compared to surgery. It is a safe, office-based procedure, which may be used on virtually any joint, ligament, or tendon of the body. Usually 3-6 monthly treatments are needed to stabilize a weak and unstable joint. Most patients have multiple joints that need treatment and each of these can be treated at the same visit. The results are generally permanent or at least last for many years after the response is initiated.
The solutions that are injected during Prolotherapy treatments have evolved over many years. The most common and extensively studied solution is a highly concentrated solution of hypertonic Dextrose, a sugar, which is mixed with local anesthetic. This has historically been mixed with other solutions and results generally show improved joint stability, ligament thickening and strengthening, and tendon-osseous junction repair. Dextrose has been proven to strengthen the connective tissue around an unstable joint and reduce pain.
More recent advances include the use of concentrated platelets from the patient’s bloodstream, a therapeutic option called Platelet Rich Plasma (PRP). The platelets contain small granules of cytokines and biological growth factors that are released into the area where they are injected. The goal of PRP is to stimulate the cells and tissues at the site of degeneration to repair and heal. Platelets appear to be suited for soft tissue repair of tears and injuries because of the higher growth factor concentrations available in the platelets as compared to Dextrose alone. Platelet Rich Plasma is often used when the degree of tissue injury is more severe. Platelet Rich Plasma is also typically more stimulating than Dextrose Prolotherapy and may require fewer treatments. Some practitioners combine PRP with Dextrose solutions at the same visit to improve results and get the combined benefits of both approaches.

Another source of growth factors and cytokines that have been extensively researched is the patient’s own Bone Marrow. Bone Marrow Aspirate Concentration (BMAC) is derived from the stem cells and growth factors present in the Bone Marrow to produce a sustained release of growth factors which help to stimulate the healing process even more powerfully than PRP alone. Experienced providers of Regenerative Medicine now are able to use combinations of Platelet Rich Plasma and Bone Marrow Aspirate Concentrate to stimulate accelerated healing for damaged tissues and strengthen the ligaments and joint capsules for the individual with Ehlers-Danlos Syndrome.
High-quality injections are usually provided using visualized guidance with fluoroscopy and ultrasound devices when necessary. The advanced regenerative medicine solutions can be precisely and safely directed to produce a greater response where the treatment is most needed.
Some individuals with Ehlers-Danlos Syndrome have very severe joint dysfunction due to their specific genetic predisposition. These patients may require more sessions of treatment, stronger concentrations of growth factors, and still may not respond as well as the typical patient.
Conclusions
Ehlers-Danlos Syndrome is a complex, frustrating condition for many people and few medical providers have extensive experience in its diagnosis and treatment. Years of patient suffering may occur before the diagnosis is appropriately made. The typical community-based treatment options for musculoskeletal pain may not reliably address the needs of an individual with EDS and may have variable results secondary to the inherent weakness of the connective tissues. Surgery may have unexpected side effects and an increased risk of failure in the population presenting with Ehlers-Danlos Syndrome.
Preservation of joint integrity and reducing the risk of serious joint injury has been the focus of this article. Regenerative Medicine using Dextrose Prolotherapy, Platelet Rich Plasma, and Bone Marrow Aspiration Concentration is proving to reliably and cost-effectively treat joint and musculoskeletal pain in those with sports-related injuries, degenerative joint conditions, and EDS population through improving the connective tissue stability and integrity. Patients suffering from chronic pain, ligament injury, tendinosis, and joint laxity associated with Ehlers-Danlos Syndrome should consider seeking consultation with an experienced Regenerative Medicine practitioner. Physical and occupational therapists can assist in the amelioration of EDS symptoms in a variety of ways but are limited in the ability to improve the osteo-ligamentous stability needed to improve joint stabilization.
Once joint integrity has been improved with the use of Regenerative Medicine techniques, the individual with Ehlers-Danlos Syndrome may see increased success with physical therapy focused on improving neuromuscular control as well as a greater tolerance to generalized conditioning and fitness program.

David Harris, MD
Board-Certified Physical Medicine
& Rehabilitation
Board-Certified Pain Medicine

Michele Harris, PT, CNP, RAS
Physical Therapist
Neurac 1 Instructor
Certified Neurac Practitioner
Resources
https://www.ehlers-danlos.com/what-iseds/
https://ehlersdanlosnews.com/prolotherapy/
https://www.ehlers-danlos.com/pdf/2018-annual-conference/L-Russek-2018Baltimore-How-Can-PT-Help-S.pdf