I wanted to take the opportunity to revisit a previous blog post dealing with an ACL tear repair using BMAC and PRP. I recently published this case report in a peer-reviewed journal (https://www.ecronicon.com/ecor/pdf/ECOR-12-00730.pdf) and we have seen several subsequent success stories in our clinic with this treatment strategy.
The anterior cruciate ligament (ACL) is a major stabilizing ligament in the knee. Rupture of the ACL (aka ACL tear) can lead to significant pain, functional deficits and accelerated joint degeneration due to knee instability.
Tissues such as cartilage, tendons and ligaments have inherent limitations in healing and regeneration. This is, in part, due to the lack of blood supply in these tissues. Subsequently, an ACL tear or rupture is not thought to heal on its own. Because of this, even small tears can lead to a chronic pain along with a change in mechanics that leads to the potential for increased tissue damage. https://charmaustin.com/where-is-your-pain/#kneepain
Surgical reconstruction is currently the gold standard for ACL tear repair. This is a valuable technique where a graft is surgically implanted in order to provide improved stability and joint protection. This treatment is not without potential consequences. This surgery often leads to impaired proprioception (how we sense where a body is in space), along with altered joint mechanics. These changes can lead to early, and accelerated, degenerative changes in the knee joint, such as arthritis.
An ACL tear does not need to be treated, but without this ligament, the knee is more unstable and this limits higher-level activities, such as sports, and also leads to increased risk of arthritis and possible need for knee replacement.
This creates a treatment gap between non-treatment and surgical ACL tear repair. More recently, use of biologic injection therapies have been proposed to help fill this treatment gap. With this strategy, injections of biologic agents, such as autologous platelet rich plasma (PRP) and/or bone marrow aspirate concentrate (BMAC), have been used to promote tissue repair in tissues that otherwise show limited ability to heal on their own.
Bone marrow is rich in several growth factors and mesenchymal stem cells. Treatment using your body’s own BMAC and PRP is a same day procedure intended to initiate the body’s natural healing processes. If repair occurs in this manner, there would be no expected alteration in joint mechanics like we see after surgery. Although there is expected post-procedure soreness after BMAC/PRP, this treatment is considered very safe and generally does not exclude other treatment options if it fails to provide significant improvements. Other advantages to treatment with BMAC/PRP include reduction of weight-bearing restrictions, as well as the need for long-term bracing and post-operative rehabilitation as seen with surgical ACL tear repair.
Surgical reconstruction remains the gold standard for ruptured ACL or ACL tear repair, however this is not without potential drawbacks. Our published case report illustrates another viable treatment option and highlights the need for further research evaluating the use of biologic treatments for orthopedic injuries such as ACL repair. Regenerative medicine treatment of ACL ruptures may help fill the treatment gap between non-treatment, or bracing alone, and surgical reconstruction.
2 MRI Comparisons of CHARM Patients’ ACL Tear Repairs
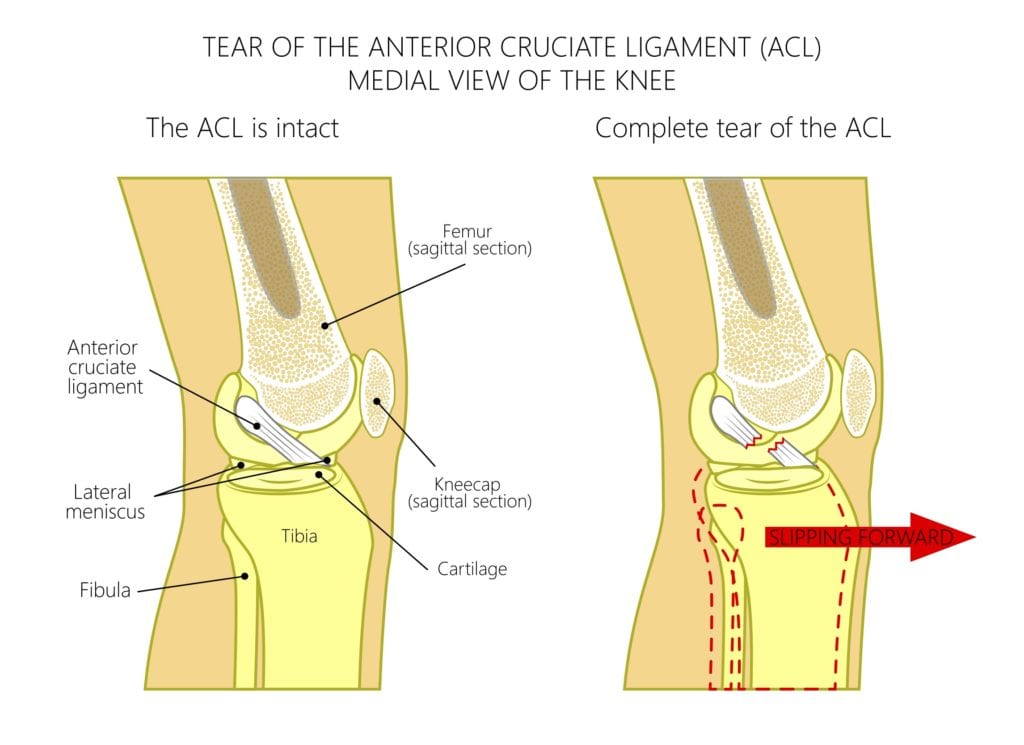
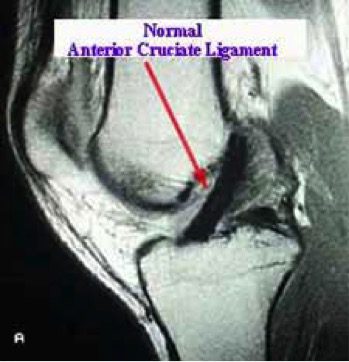
The above vector image and MRI scan show what a normal intact ACL looks like. The vector image also depicts what a a rupture or tear looks like. You will see MRI imaging or patient’s injury prior to treatment and MRI imaging of patient’s results of repair post treatment at CHARM with Platelet Rich Plasma (PRP) and Bone Marrow Aspirate Concentrate (Stem Cell Therapy).
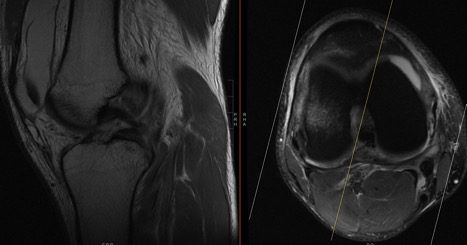
CHARM Patient #1 ACL Tear
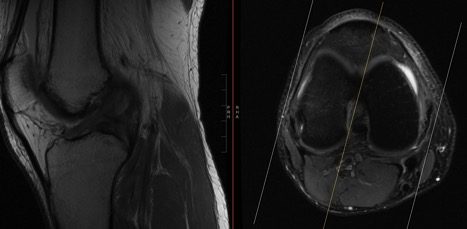
CHARM Patient #1 ACL Post Treatment
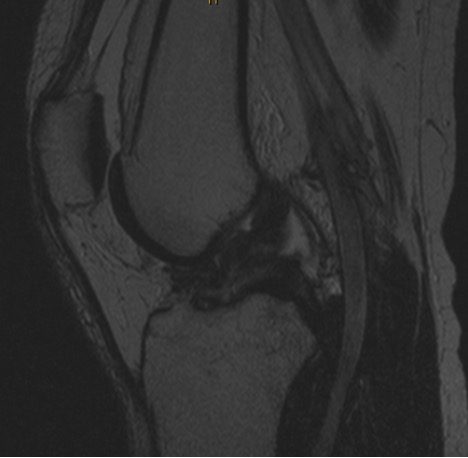
CHARM Patient #2 ACL Tear
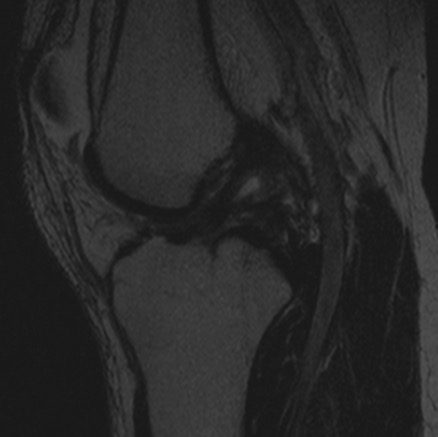
CHARM Patient #2 ACL Post Treatment
Ben Rawson, D.O. https://charmaustin.com/why-charm/the-charm-team/ben-rawson-do/

