
Do you struggle to not wobble, feel dizzy or stay steady and if so, how can you achieve better balance? Balance is the ability of an individual to control their center of gravity in order to remain upright. It is context specific, meaning balance is influenced by the environment, the person, and the task. Every person should be able to recover their balance when faced with a sudden obstacle and be able to adapt to changing balance requirements.
Many people believe that good balance is simply something that comes naturally to us when we are young and declines as we age. In reality, good balance requires appropriate functioning of 3 different body systems and can be trained and improved. In older adults, balance becomes especially important to reduce the risk of falls and possible resulting injuries, such as hip fractures, concussions, and severe bruising.
3 Body Systems to Train for Better Balance
The 3 systems that make up balance are the somatosensory, visual, and vestibular systems. These systems work together to help us remain upright, recover balance, and adapt to changing environmental conditions.
The somatosensory system involves the perception of touch, pressure, position, and movement, specifically of the feet and ankles. Imagine you are walking on a rocky surface; your somatosensory system is being used to sense the rocks underneath your feet and changes the position and movement of your feet and ankles, so you don’t fall.
The visual system involves using eyesight to take in your environment and detect obstacles that may cause you to lose your balance. For example, if you are walking up the stairs in the dark, you may not perceive the last step which can result in losing your balance and needing to grab on to a rail to prevent a fall.
Lastly, the vestibular system involves the structures of the inner ear and provides the brain with information about where your head, eyes, and body are in relation to gravity. This system generates compensatory movements to help maintain stability of the head and body in space. To illustrate, if you roll over quickly in bed and begin to experience dizziness, the vestibular system will work to reorient your brain to the position of your body in space, and the dizziness should go away.
Balance can also be affected by the state of the musculoskeletal system. Appropriate muscle strength, mobility of joints, and intact sensation are all a part of being able to maintain balance. For example, if the muscles of the hips and legs are weak, a trip over a small curb could result in a fall since the muscles are not able to engage to keep your body upright. Physical therapists are trained to address muscle weakness, joint motion, and altered motor control of the extremities, all of which can improve balance and decrease the risk of falls. For more information about PT at CHARM click here: https://charmaustin.com/restore-function-and-return-to-living/
Falls Can Happen Without Proper Balance
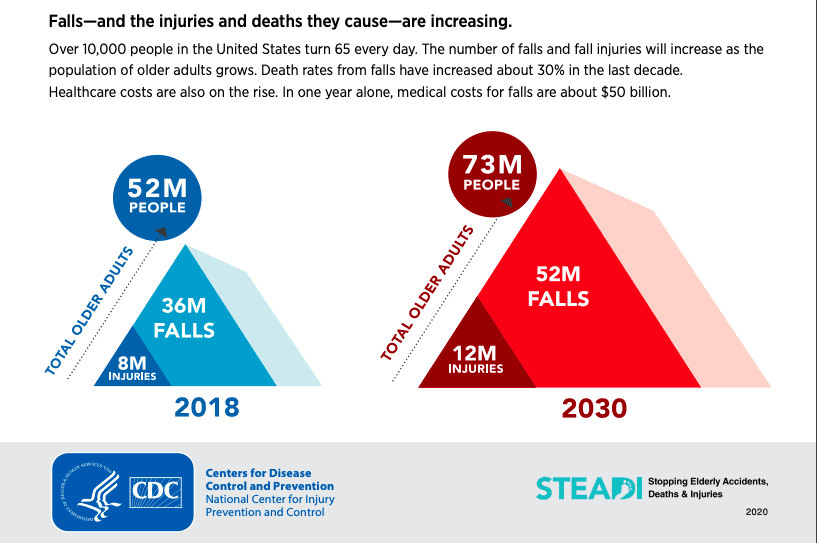
A fall can be defined as an event that results in an individual unexpectedly coming to rest on the ground or a lower surface without a loss of consciousness. Over 1/4 of people over the age of 65 fall each year, and in 2018 there was an estimated $50 billion dollars spent on medical expenses related to falls. It is important to recognize that falling, and even fear of falling, are not a normal part of the aging process.
There are steps that can be taken to decrease the risk of falls, addressing both intrinsic and extrinsic factors.
Examples of intrinsic risk factors include:
- Muscle weakness
- Decreased joint mobility
- Poor reaction time
- Fear of falling, history of falls
- Impaired sensation
- Dizziness
Examples of extrinsic risk factors include:
- Taking more than 4 medications
- Poorly fitting footwear
- External hazards (rugs, cords, etc.)
- Wet/slippery floors
- Poor lighting
- Clutter
Better Balance and Fall Prevention
Effective fall prevention requires addressing both intrinsic and extrinsic factors. If you have fallen or are afraid of falling, you should tell you doctor. They can assess your eyesight, medication list, and associated medical conditions, such as osteoporosis, that may increase your risk for falls, and make adjustments accordingly. They may also refer you to a physical therapist to address other intrinsic risk factors such as muscle weakness, decreased joint mobility, and poor reaction time. In terms of extrinsic risk factors, here are some simple guidelines to follow:
- Get rid of trip hazards around your home; this includes throw rugs, long cords, and clutter
- Use handrails when going up and down stairs
- Ensure the area where you are walking is well-lit
- Use non-slip mats in showers/bathtubs
For more information about how to prevent falls visit the CDC’s website to learn about their STEADI (Stopping Elderly Accidents, Deaths and Injuries) program.

Catherine Madsen, PT, DPT
