All too often we hear the common scenario of being in a hurry and falling off of a ladder, slipping on wet floors or falling on ice. These typically lead to the onset of mid to lower back pain. One of the most common consequences of falls in middle to older adults is compression fracture(s) that can occur at one or more levels of the mid back or thoracic spine or upper lumbar spine region.
What is a Compression Fracture?
A compression fracture occurs when a part of the spine, the block shaped anterior part of the bone that stacks on one another forming the column of the spine, collapses. There are several types of these fractures including crush, burst and wedge fracture. Wedge compression fractures usually occur along the anterior or front of the vertebrae.
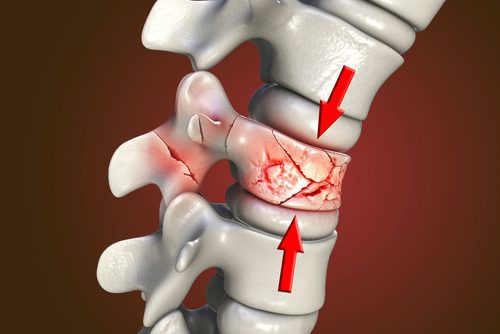
3D Illustration of a Spinal Compression Fracture 
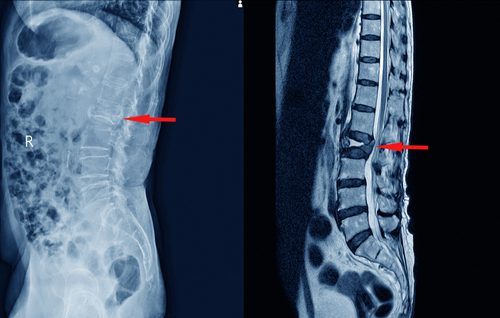
Patient MRI showing Compression Fracture
Who is at Risk for These?
Compression fractures are most common in the elderly and affect 25% of post menopausal women in their lifetime. That number increases with age. The patients at highest risk have osteoporosis, a condition in which bones become weak and brittle. Other risk factors include previous trauma and cancer.
Having a history of one compression fracture increases the risk for future vertebral fractures of the same kind. The majority of compression fractures occur in the Thoracolumbar region between T12 and L2 which is a transition zone from the rigidity of the thoracic spine to the more flexible lumbar spine. Evaluation and Management of Compression Fractures
What Can Cause These Types of Injuries?
Elderly patients with Osteoporosis are at increased risk of compression fractures from trivial events including lifting an object, falling off of a chair, or rolling over in bed. Other causes of compression fractures include falls, trauma ie. fall from a height or motor vehicle accident.

Signs and Symptoms
The most common complaint is mid to low back pain commonly after a fall or injury that increases with standing and walking and is decreased with laying down. There is pain with decreased spinal mobility.
Are you at Risk for Compression Fractures?
There are many factors that increase your likelihood for these, the most common among them is Osteoporosis. Other risk factors for compression fractures that can be changed with lifestyle modifications include low Vitamin D levels, Calcium Deficiency, alcohol consumption, tobacco use, poor eyesight and low body weight.
Prevention
There are many practical ways to reduce your risk factors.
- Vitamin D Supplementation, most people can easily take 5,000 IU/day of this fat loving vitamin that helps maintain bone and joint support.
- Calcium/ Dairy intake: Making sure to take calcium supplements is an option and j1200 mg/day is recommended. The easiest way to obtain this supplement is through dietary intake, including yogurt, dairy, cheese. Non dairy sources rich in calcium include deep green leafy vegetables, beans, kale, and almonds to name a few.
- Men should be tested for low Testosterone
- Daily weight bearing exercise is an important way to increase bone density and reduce risk for osteoporosis.
- Medications: Bisphosphonates are oral medications prescribed in patients’ with Osteopenia or low bone density and reduce risk for fractures.
How are These Particular Fractures Treated?
Non surgical treatment includes analgesic and non steroidal anti inflammatory medications including Ibuprofen, and occasionally in severe cases narcotic pain medications can be used on a limited basis for short term only.
In cases of significant vertebral body compression, treatment with procedures called Vertebroplasty where cement is injected into the vertebral body or Kyphoplasty where a balloon inflates the height of the vertebral body can be used to reduce pain and improve patient function and mobility.

Michelle Hall
PA-CPhysician Assistant